
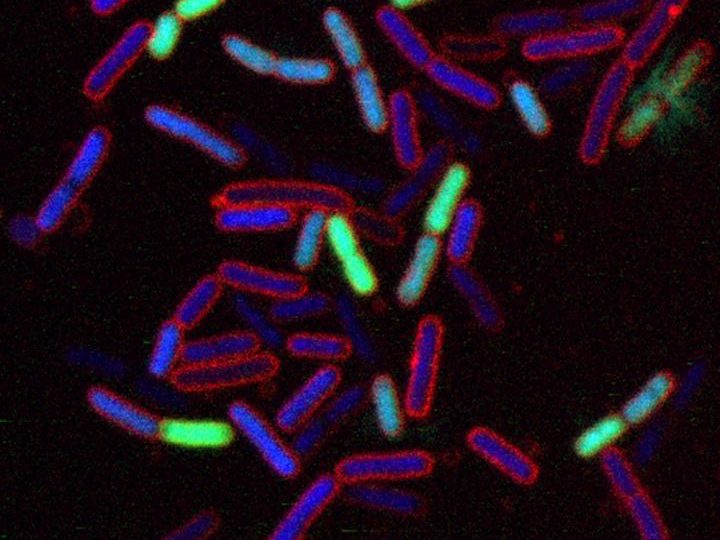
Escherichia coli cells treated with a novel chimeric peptidomimetic antibiotic. Cells in blue are alive while green cells are already killed by the peptidomimetic. As the antibiotic destroys the integrity of the bacterial membranes, we observed ‘explosive cell lysis’ (cells indicated by arrows), which leads in the release of DNA (diffuse green). ©Matthias Urfer, UZH.
(Anatol Luther et. al. Chimeric Peptidomimetic Antibiotics Against Gram-Negative Bacteria. Nature. 23 October 2019. DOI: 10.1038/s41586-019-1665-6)
A new puzzle to be solved
Furthermore, a recent research led by a scientist at City University of Hong Kong (CityU) has discovered a plasmid that can make a new type of hyper-resistant and deadly superbug become hyper-virulent quickly, posing an unprecedented threat to human health. In 2017, Professor Chen Sheng, who then worked at the Hong Kong Polytechnic University, together with his research team and collaborators from Zhejiang University, discovered a new strain of Klebsiella pneumoniae which was not only resistant to carbapenem, but also hyper-virulent and highly transmissible. Their findings were published in Lancet Infectious Diseases (DOI: 10.1016/s1473-3099(17)30489-9). “But we did not know how this superbug was formed,” said Professor Chen, who is now the Acting Head of Department of Infectious Diseases and Public Health at City University of Hong Kong. Recently, when Professor Chen and his team isolated a carbapenem-resistant Klebsiella pneumonia strain from a patient in a Chinese hospital, the phylogenetic analysis revealed that the strain actually belonged to Klebsiella variicola strain. “Klebsiella variicola was rarely isolated from clinical samples. It usually resides in the respiratory and gastrointestinal tract of patients without producing typical signs of bacterial infections,” said Professor Chen. Its team discovered that this strain actually carries a new conjugative plasmid which harbours the key genes of the virulence plasmid commonly found in hyper-virulent Klebsiella pneumoniae, leading to high-level virulence and making the bacteria more dangerous. In the experiments, when the mice were infected with carbapenem-resistant Klebsiella pneumonia with this plasmid, all the mice died, and the mortality rate was similar to the hyper-virulent control strain. But when the mice were infected with the same strain which lacked this plasmid, all of the mice survived. Further experiments also discovered that the new-found plasmid could travel from one bacterium to another. The transfer of this virulence plasmid to a carbapenem-resistant Klebsiella pneumoniae strain can result in a significant increase in the virulence level of such strain, making it both carbapenem-resistant and hyper-virulent. “ This suggests that the hyper-virulent Klebsiella pneumoniae, which can cause a deadly infection in humans, could become prevalent due to the transmission of this plasmid in clinical Klebsiella pneumonia and pose a bigger threat to patients’ health,” said Professor Chen. Based on this finding and more data from his team, Professor Chen said that there would be more different types of conjugative virulence plasmid transmitting around in clinical Klebsiella pneumoniae. His team will continue to investigate more clinical Klebsiella penumoniae strains to discover more different types of conjugative virulence plasmids, which attribute to the current emergence of hypervirulent and carbapenem-resistant Klebsiella pneumoniae. The new findings were published in Nature Microbiology (DOI: 10.1038/s41564-019-0566-7. A conjugative plasmid that augments virulence in Klebsiella pneumoniae. Xuemei Yang, Edward Wai-Chi Chan, Rong Zhang & Sheng Chen).



COMMENTS ARE OFF THIS POST